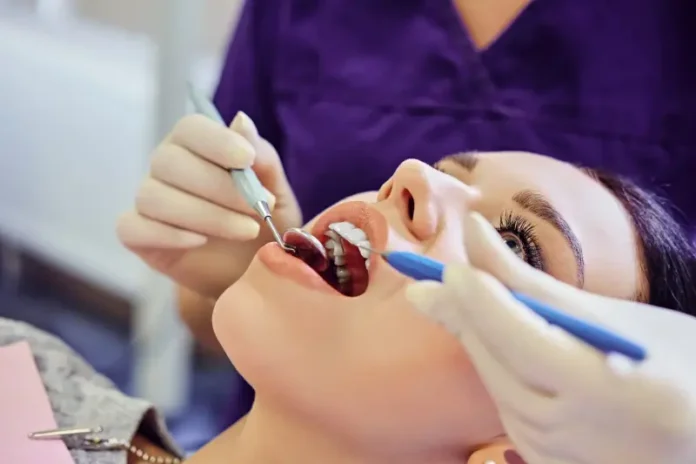
Oral health can provide an early indication of a broad range of health conditions but these signs are often missed by primary care physicians. A new report from the United States Preventive Services Task Force on primary care and prevention found that regular dental screenings at primary care facilities tend to overlook many dental conditions.
The new finding is worrisome not only to the health authorities but also to individual patients, as some of these medical conditions are not only indicative of poor oral health but could also be an early-warning sign of other medical concerns.
Given the heavy workload on many primary care physicians, it is understandable that they do not find time to examine oral health in greater detail. Even when they do check the mouth, it is more likely they are looking at the throat area rather than examining dental health. Dentists are urging primary care doctors to pay closer attention to signs of illness that may show up in the mouth first, or to refer the patient to a professional dentist at the earliest signs of oral concern.
Dentists point out that treating gum and other oral diseases early on, as well as maintaining good oral health habits can not only improve dental health but also could prove to be beneficial from an overall health perspective. Some of the key conditions that dentists would like primary care physicians to pay greater attention to during regular checkups, in order to treat dental diseases early on, as well as to help detect other associated diseases, include:
Diabetes: The oral health realm can leave a distinct imprint of type 2 diabetes (T2D) that dental professionals are trained to watch for. For example, gum disease, which is marked by inflamed, bleeding gums, can be an early sign of T2D. People with diabetes may also have a dry mouth, stemming from reduced production of saliva, leading to discomfort, a hard time swallowing, and a higher risk of dental infections.
On average, around 43 percent of people with diabetes have dry mouth.
Another sign that can show up in the mouth is oral thrush, a fungal infection in the mouth. Although it is not contagious and is usually treated with antifungal medication, oral thrush, also called oral candidiasis, which appear as creamy white lesions on the tongue or inner cheeks, could be a sign of reduced immunity and also of uncontrolled diabetes.
Inflammatory bowel disease (IBD): Intestinal illnesses like Crohn’s disease and ulcerative colitis have long been recognized for their effect on the overall health of individuals. However, a lesser-known aspect of these disorders is their potential to show up in the mouth, presenting a unique set of challenges for both patients and health care providers. Some people with IBD have painful ulcers in the mouth that are commonly known as canker sores, or as aphthous stomatitis by doctors. These oral symptoms not only add to discomfort for those with IBD, but also can show that a disease is present.
These ulcers are typically seen on the soft tissues lining the mouth, such as the inner cheeks, lips, and tongue. IBD and oral ulcers come with inflammation. The body’s immune response can result in an overproduction of cytokines — small proteins that are crucial in controlling the growth and activity of other immune system cells and blood cells — that trigger a cascade of proinflammatory events that could lead to formation of painful ulcers.
Heart disease: The mouth may be an unexpected place to find early signs of heart and blood vessel diseases, but new research now shows that gum diseases and other oral symptoms could be an early sign of heart related issues. The connection lies in the inflammatory nature of both conditions; chronic heart disease may add to an inflammatory response that, in turn, worsens gum inflammation and leads to more severe issues with the teeth and gums.
Symptoms such as bleeding gums, persistent bad breath, and gum swelling can serve as early warning signs. People with gum disease are also at a higher risk of having issues with their heart and blood vessels, and bacteria in the mouth can enter other areas of the body, including the heart.
Osteoporosis: Osteoporosis, a bone disease that leads to fractures and disability, often goes unnoticed until the condition leads to injury. But research shows it can affect the teeth in noticeable ways, including tooth loss and gum disease. Moreover, some of the medications prescribed for osteoporosis, such as bisphosphonate drugs,can cause dental issues such as dry mouth and tooth decay. This is something that doctors may not be aware of when prescribing these medications.
Oral cancer: Symptoms of oral cancer that may be visible during a primary health care visit include a sore on the lip or in the mouth, white or reddish patches on the inside of the mouth, loose teeth, or a lump inside the mouth.
Experts are now recommending a biopsy anytime a doctor finds a white patch in the mouth that the patient has not had before and which persists for over two to three weeks.Human papillomavirus (HPV) — a common virus infection that may cause cancers later in life — has been linked to oral cancers, including oropharyngeal cancer found in the throat.
Compared with other cancers, oral and pharyngeal cancer has one of the poorest five-year survival rates: only 52 percent of people diagnosed with oral cancer survive five years, while only 35 percent of oral cancer is detected at the earliest stage. Doctors point out that most oral cancer patients are diagnosed at an advanced stage of the disease, which accounts for the higher mortality figures.
It is also worth underlining that while some health issues may show up in the mouth, the problems go both ways: Poor oral hygiene can lead to negative health outcomes. Going to the dentist regularly, brushing at least twice a day, flossing at least once a day, all of these things can contribute to not only better oral health but also greater overall health.